The Recovery Debt That Accumulates Shift by Shift
There is a number that should stop every nurse and healthcare worker cold: musculoskeletal conditions cost affected adults several thousand dollars annually in out-of-pocket and total healthcare expenditures, and those with chronic back conditions pay significantly more, according to AHRQ's Medical Expenditure Panel Survey (MEPS). For a profession that exists to absorb the healthcare costs of others, nurses and hospital workers are quietly running up a substantial tab of their own - paid in pain, sleep debt, and medication dependence that too often becomes the default recovery strategy.
This is not a wellness trend story. This is a data story about a specific occupational health problem - one that federal agencies have been documenting for years - and a non-pharmacologic recovery intervention that a growing body of research, including NIOSH-cited literature, now supports as legitimate adjunct therapy. Cold-water immersion is not a cure. It is one evidence-informed tool in a recovery stack that healthcare workers are building because the alternative - doing nothing - has a documented physiological and financial cost.
Why Healthcare Workers Break Down: The Biomechanical and Physiological Mechanism
Understanding why nurses accumulate musculoskeletal damage faster than nearly any other profession requires understanding what a 12-hour hospital shift actually does to a body.
Hospital floors are unforgiving surfaces. Nurses spend the majority of a shift on their feet on hard linoleum or tile, performing patient transfers that can require exerting 35 to 100 pounds of force per assist, bending and twisting at the lumbar spine thousands of times per week, and sustaining cognitive load that keeps the sympathetic nervous system - the stress-response system - chronically activated. This matters for recovery because a chronically activated sympathetic nervous system suppresses the parasympathetic processes that facilitate actual tissue repair: growth hormone release, protein synthesis, and inflammatory resolution.
When muscles are repeatedly loaded without adequate recovery, the body produces creatine kinase (CK) - an enzyme released from damaged muscle fibers - and accumulates inflammatory cytokines like interleukin-6 and tumor necrosis factor-alpha. These are the biomarkers associated with delayed-onset muscle soreness (DOMS), the stiffness and aching that peaks 24-72 hours after intense physical exertion. For nurses working back-to-back shifts, this recovery window is often nonexistent. The damage from Monday's shift hasn't resolved by Wednesday's shift. Over months and years, this is the architecture of a musculoskeletal disorder.
Beyond the musculoskeletal load, there is the cardiovascular dimension. CDC WONDER data tracks that cardiovascular disease accounts for approximately 1 in 3 U.S. deaths annually. Chronic occupational stress - the sustained sympathetic activation that healthcare workers experience - is an established risk factor for cardiovascular disease progression. The intersection of physical overload and psychological stress in nursing is not incidental; it is structural.
Cold-water immersion addresses several of these mechanisms simultaneously. NIOSH-cited recovery research documents that cold-water immersion at 50-59°F (10-15°C) for 10-15 minutes post-exertion reduces delayed-onset muscle soreness and lowers serum creatine kinase markers - the precise biomarkers elevated by the kind of repetitive patient-handling and prolonged standing that defines nursing work. The cold drives vasoconstriction, which reduces inflammatory edema in loaded tissues, then triggers vasodilation upon rewarming, flushing metabolic waste. It also produces a measurable shift toward parasympathetic dominance - the nervous system state associated with rest, recovery, and tissue repair - which may explain why regular cold immersion practitioners report improvements in perceived stress and sleep quality.
This is not fringe science. This is the physiological rationale that has led occupational therapists and sports medicine physicians to recommend cold immersion protocols to workers in physically demanding occupations - and why nurses are searching for home cold plunge units at an accelerating rate.
The Cheapest Intervention Is the One That Doesn't Require Buying Anything
Before we get to equipment, this section matters most. No cold plunge - regardless of price - compensates for the foundational recovery behaviors that are free, evidence-anchored, and available tonight. Federal occupational health guidance consistently positions these as the first line of intervention for workers accumulating physical and psychological stress load.
NIOSH-validated work-rest cycles are the structural fix that cold immersion gets layered on top of, not a substitute for. For physically demanding work under heat or load, NIOSH recommends scheduled rest in cool environments - and advocates for pacing the work itself as the primary prevention strategy. If you are scheduling cold plunges but not advocating for adequate break time in your facility, you are treating the symptom rather than the exposure.
Active recovery over passive rest is the second principle that changes outcomes before any equipment enters the picture. CDC physical activity guidance underscores that 10-15 minutes of light walking or low-intensity cycling after intense physical work clears blood lactate significantly faster than sitting still. Active recovery is the foundation; cold immersion is the accelerant on top of it.
Hydration is non-negotiable and frequently neglected on busy hospital floors. CDC NIOSH heat-related illness guidance recommends one cup (8 oz) of water every 15-20 minutes during physical exposure, with electrolyte replacement on shifts longer than two hours. Cold immersion does not replace fluid loss. Arriving at a cold plunge dehydrated blunts its benefits and increases cardiovascular risk.
Sleep is the recovery multiplier that no product replaces. CDC guidance is clear: adults need 7 or more hours of sleep per night, and sleep deprivation directly increases workplace injury rates. If a nurse is running on 5-6 hours between shifts, a cold plunge improves nothing systemically. The sequencing is: adequate sleep first, structured active recovery second, cold immersion third.
For readers who have addressed the fundamentals above - who are sleeping adequately, hydrating well, incorporating active recovery, and still finding that the cumulative physical load of healthcare work is outpacing their body's ability to repair - this is where targeted recovery equipment becomes a legitimate conversation. Cold immersion is not a biohack or a luxury wellness trend in this context. It is a documented physiological intervention for reducing the specific biomarkers elevated by your occupational exposure.
When to See a Clinician Before Starting Cold Immersion
Cold-water immersion is contraindicated for a meaningful subset of healthcare workers, and the irony is that the same occupational stressors that make nurses candidates for cold therapy also elevate their cardiovascular risk profile. This is a clinical conversation, not a consumer one.
NIH's National Heart, Lung, and Blood Institute documents that cold-water immersion can trigger acute cardiovascular events in individuals with hypertension, arrhythmias, Raynaud's phenomenon, or recent cardiac history. The cold-shock response - an involuntary gasp reflex and acute sympathetic surge triggered by sudden cold immersion - can precipitate dangerous heart rhythm changes in susceptible individuals. Given that cardiovascular disease accounts for approximately 1 in 3 U.S. deaths annually per CDC WONDER data, and that healthcare workers carry elevated cardiovascular risk due to chronic stress exposure, this is not a theoretical concern.
Seek clinical clearance before beginning cold immersion if any of the following apply:
- You have diagnosed or suspected hypertension, even if controlled with medication - cold immersion acutely elevates blood pressure and heart rate
- You have any history of cardiac arrhythmia, including atrial fibrillation or SVT
- You have Raynaud's phenomenon or any condition involving abnormal peripheral vascular responses to cold
- You have had a cardiac event, procedure, or hospitalization within the past 12 months
- You are pregnant
If none of these apply, starting conservatively - water at 60°F, immersion for 3-5 minutes, with a partner present - is the evidence-consistent approach before progressing to the 50-59°F range documented in NIOSH-cited literature.
Where Products Enter the Recovery Stack
For healthcare workers who have cleared the clinical checklist and are ready to build a consistent cold immersion protocol at home, equipment matters - but in a specific way. You are not buying a wellness gadget. You are buying a tool that determines whether you can sustain a recovery protocol consistently, which is the variable that actually produces physiological adaptation.
Consistency requires convenience. A cold plunge that requires 45 minutes of setup and 30 lbs of ice per session will be used twice and abandoned. A unit that is ready within a temperature range and requires minimal maintenance will be used three to four times per week - which is the frequency range where NIOSH-cited recovery literature shows measurable CK reduction.
For nurses who want to enter cold immersion without a four-figure equipment commitment, the Ice Barrel 400 is the most honest starting point in this category. At $1,200, it is a vertical-immersion barrel designed without a chiller - you cool it with ice, drain, and refill. That sounds like a limitation, but for a nurse using it two to three times per week in a climate with seasonal variation, ice cost is manageable and the upright ergonomic position actually reduces lumbar strain during entry and exit compared to lying flat in a tub. The barrel design also means it stores in a garage or on a small patio without significant footprint. This is the best-fit option for a healthcare worker doing their first year of cold immersion who wants to validate whether the protocol works for their body before spending more.
For nurses who have already validated the protocol and are dealing with the friction of ice logistics - or who are using cold immersion five to seven times per week as a serious recovery tool - the Sun Home Cold Plunge Pro solves the maintenance problem that eventually ends most ice-based protocols. At $4,499, it is a self-cleaning, chiller-equipped unit that maintains a target temperature (down to the 50-59°F range documented in NIOSH recovery literature) without ice management. For a nurse who just finished a 12-hour shift and has approximately 20 minutes of functional decision-making energy left, a unit that is ready at temperature and requires no setup is the difference between completing a recovery session and not. The self-cleaning filtration system also matters for healthcare workers specifically: you are already working in environments with high pathogen exposure. The last thing a nurse needs is to add a poorly maintained water vessel to their home environment.
Cold Plunges Built for Healthcare Worker Recovery: Evaluated for Shift Fatigue, Maintenance Overhead, and Temperature Precision
These two units were evaluated specifically for the constraints nurses and healthcare workers face: limited post-shift energy for maintenance, need for consistent temperature in the 50-59°F range documented in NIOSH recovery literature, and ergonomic entry and exit that does not add lumbar strain to an already-loaded spine.
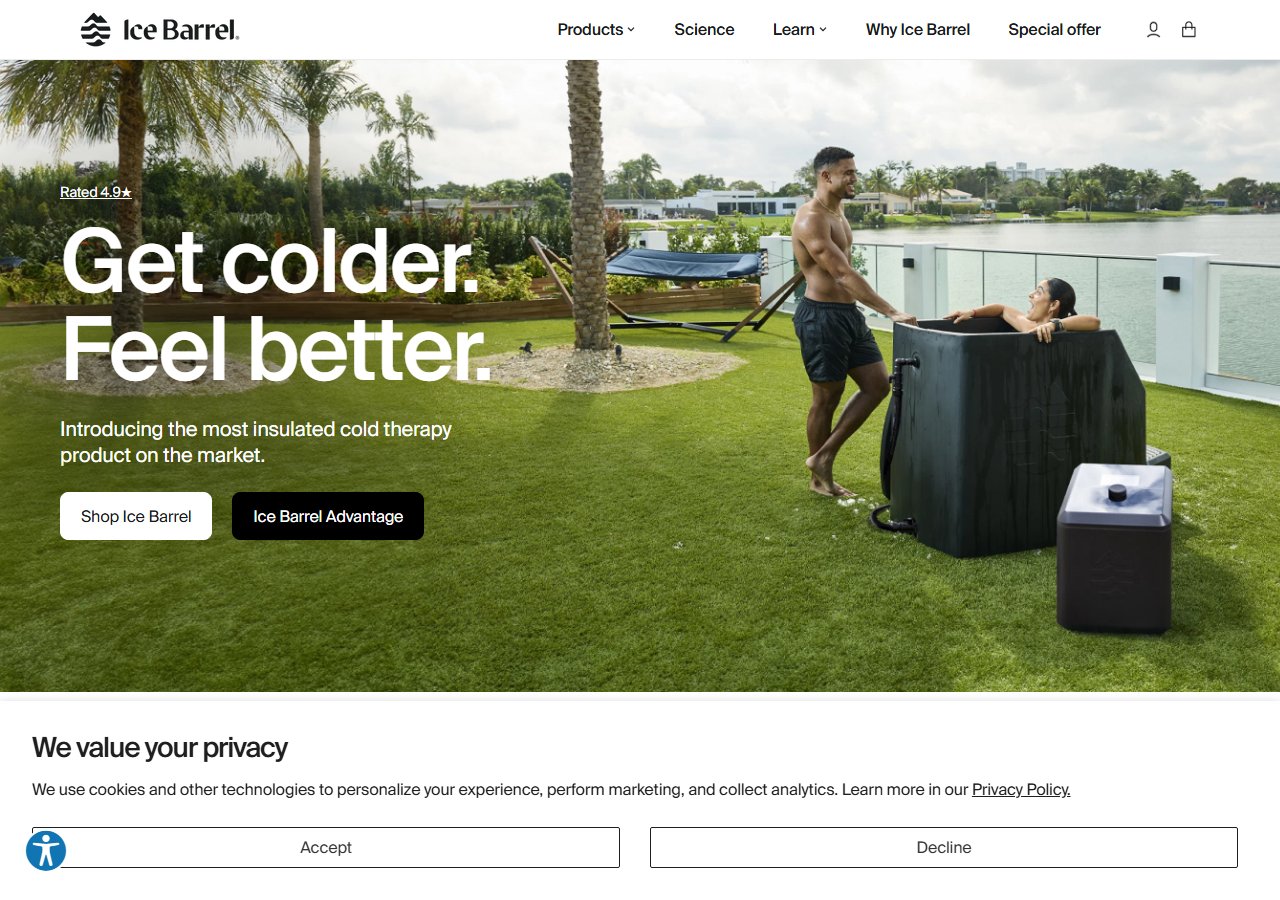
Ice Barrel 400
$1,200
See Price at Ice Barrel →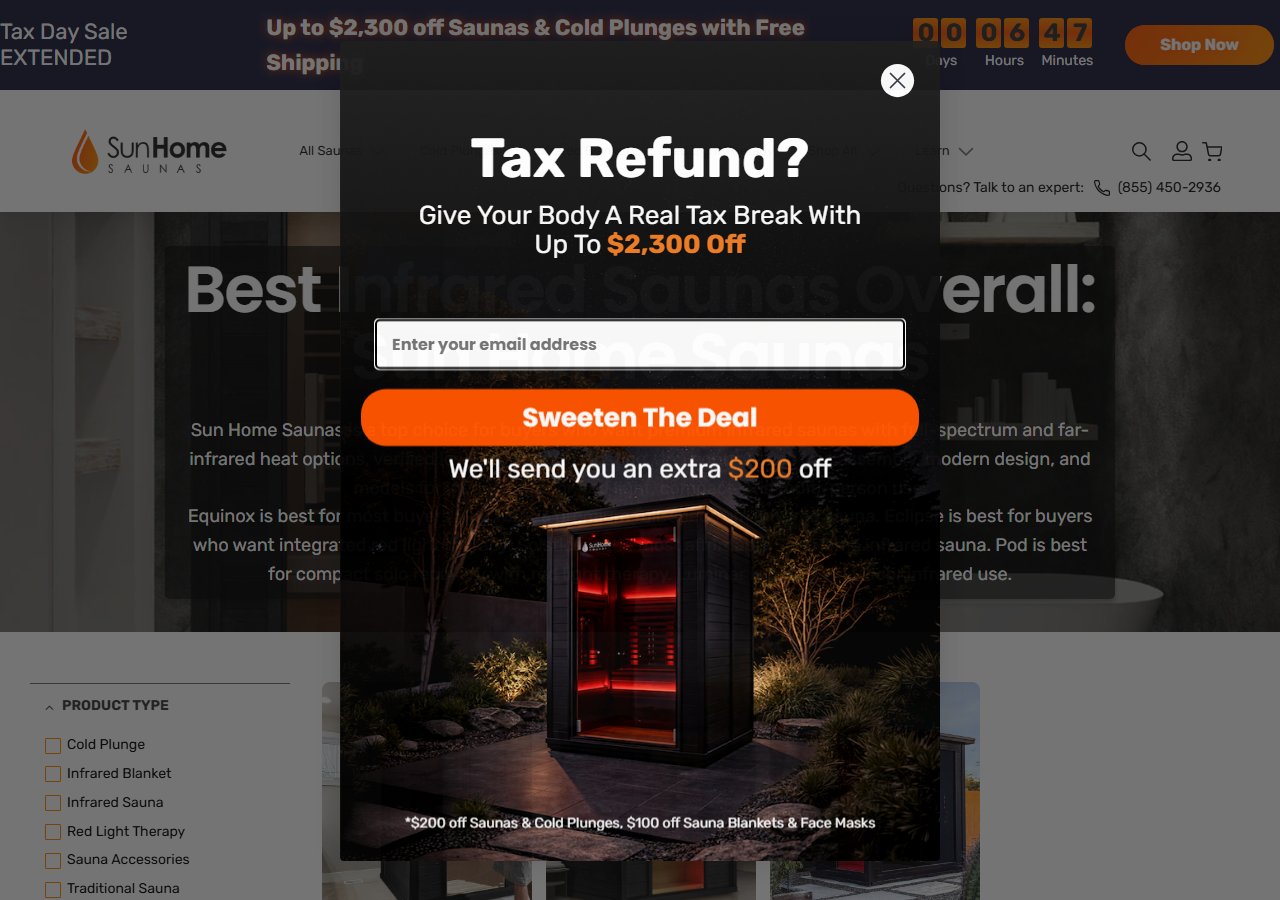
Sun Home Cold Plunge Pro
$4,499
See Price at Sun Home →The Financial Case for Prevention: MEPS Data in Context
The question nurses often ask when evaluating a $1,200 or $4,499 cold plunge is whether it is a justifiable expense on a nurse's salary. The AHRQ MEPS data provides a useful anchor. Per-person healthcare expenditures for musculoskeletal conditions average several thousand dollars annually for affected adults - and that figure rises significantly for chronic back conditions, which are among the most common occupational injuries in nursing. A single year of chronic back-related healthcare costs - imaging, physical therapy copays, medications, lost wages from missed shifts - can easily exceed the cost of the recovery equipment being discussed here.
This is not a claim that a cold plunge prevents musculoskeletal disorders. It is a claim that a consistent, evidence-informed recovery protocol - anchored in the interventions described earlier in this article and augmented by cold immersion where appropriate - represents a physiologically rational investment in preventing the accumulation of damage that eventually produces the conditions MEPS is tracking.
BLS CFOI data from 2024 documents that construction workers logged 1,075 fatal work injuries in 2023, the highest of any private industry sector - a figure cited here not because nursing carries equivalent fatal injury risk, but because it illustrates the principle that occupational physical exposure has quantifiable consequences, and that those consequences are tracked, documented, and real. Healthcare workers occupy a different part of the BLS injury landscape - one characterized by higher rates of musculoskeletal disorders, needlestick exposures, and violence-related injuries - but the underlying principle is identical: the body accumulates the exposure, and recovery infrastructure is what determines whether that accumulation produces long-term damage.
The Bottom Line for Healthcare Workers
Cold immersion is not magic. It is a documented physiological intervention - grounded in NIOSH-cited recovery research - that reduces the specific biomarkers elevated by the kind of physical and psychological load that nursing produces. It works best as one component of a recovery stack that starts with adequate sleep, hydration, and active recovery, and is deployed after clinical clearance in anyone with cardiovascular history.
For nurses who have done the foundational work and are ready for equipment: the Ice Barrel 400 is the honest starting point at $1,200, and the Sun Home Cold Plunge Pro is the serious long-term tool at $4,499. Both are matched to the specific recovery needs of healthcare workers - the ergonomic entry, the maintenance overhead relative to shift fatigue, the temperature precision that the federal recovery literature specifies.
Your patients need you functional for decades. That requires treating your own recovery with at least a fraction of the clinical seriousness you apply to theirs.